all-in-one billing solution
Are you overwhelmed with your medical billing?
Let Clarity Billing handle it from A-Z

Expertise & Experience

Customized Solutions

Efficiency & Time Savings

Maximize Revenue

Accuracy & Compliance
Financial Success
At Clarity Billing, we believe in a partnership approach. We’ll work closely with your team to understand your practice’s unique needs and tailor our services accordingly. Your success is our success, and we’re dedicated to helping you achieve your financial goals while providing exceptional patient care.
Our Services
Patient Demographics
Our skilled billing team is responsible for entering charges accurately. Our dedicated Data Entry and Quality Control teams ensure that all information is entered correctly as provided. We understand how crucial it is to accurately input insurance ID numbers, claims addresses, patient demographics and all insurance information details. This accuracy directly affects how claims are processed and payments are made.

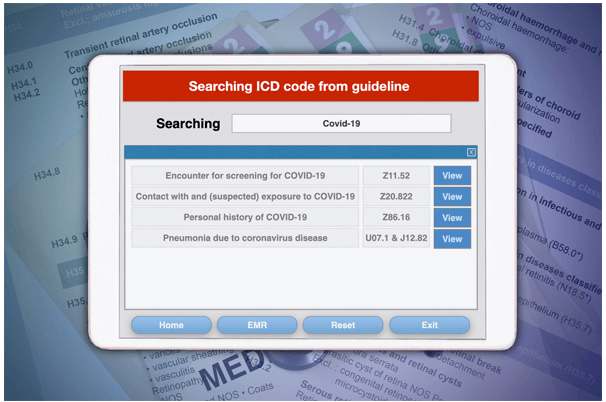
Coding
Our billing team is knowledgeable about working with different medical specialties. They understand how to connect the right CPT codes to diagnosis codes to make sure claims are paid correctly. Our team is also familiar with using various medical billing software. This helps us start working without delay, saving time and effort on staff training.
Payment Posting
We have skilled and trained billing experts who understand various types of EOBs from all insurance providers. They handle both manual and electronic payment postings. Payments from patients and insurance companies are accurately recorded in the client’s medical billing system. To ensure accuracy, these recorded payments are compared to the bank deposit slips on a daily basis.


Denials
Our skilled team dedicated to handling claim denials takes a thorough look at your remittance advice. They pinpoint why denials, zero payments, and claim reversals happen, and then work diligently to resolve these issues until the claims are successfully resolved.
A/R Follow-Up
Getting paid for the services a medical practice provides is crucial, but it’s a challenging job. At Clarity Billing, our skilled professionals use effective methods to recover the money owed. We use specialized software to keep track of outstanding payments and communicate effectively with insurance companies to ensure successful collection.


Provider Credentialing
Becoming a part of a payor network and boosting revenue is a big deal. Our experienced team takes care of this crucial process. They carefully review documents, fill out forms, and manage the credentialing for providers, ensuring they can join the network successfully.
Eligibility & Benefits
Offering a pre-appointment benefit check service can greatly improve a doctor’s office efficiency. By obtaining eligibility and benefits information beforehand, the administrative process becomes smoother, minimizing billing surprises and allowing the medical staff to concentrate on patient care. Patients will value the upfront clarity about their financial responsibilities, leading to a positive experience.

Our Services
Patient Demographics
Our skilled billing team is responsible for entering charges accurately. Our dedicated Data Entry and Quality Control teams ensure that all information is entered correctly as provided. We understand how crucial it is to accurately input insurance ID numbers, claims addresses, patient demographics and all insurance information details. This accuracy directly affects how claims are processed and payments are made.

Coding
Our billing team is knowledgeable about working with different medical specialties. They understand how to connect the right CPT codes to diagnosis codes to make sure claims are paid correctly. Our team is also familiar with using various medical billing software. This helps us start working without delay, saving time and effort on staff training.

Payment Posting
We have skilled and trained billing experts who understand various types of EOBs from all insurance providers. They handle both manual and electronic payment postings. Payments from patients and insurance companies are accurately recorded in the client’s medical billing system. To ensure accuracy, these recorded payments are compared to the bank deposit slips on a daily basis.

Denials
Our skilled team dedicated to handling claim denials takes a thorough look at your remittance advice. They pinpoint why denials, zero payments, and claim reversals happen, and then work diligently to resolve these issues until the claims are successfully resolved.

A/R Follow-Up
Getting paid for the services a medical practice provides is crucial, but it’s a challenging job. At Clarity Billing, our skilled professionals use effective methods to recover the money owed. We use specialized software to keep track of outstanding payments and communicate effectively with insurance companies to ensure successful collection.

Provider Credentialing
Becoming a part of a payor network and boosting revenue is a big deal. Our experienced team takes care of this crucial process. They carefully review documents, fill out forms, and manage the credentialing for providers, ensuring they can join the network successfully.

Eligibility & Benefits
Offering a pre-appointment benefit check service can greatly improve a doctor’s office efficiency. By obtaining eligibility and benefits information beforehand, the administrative process becomes smoother, minimizing billing surprises and allowing the medical staff to concentrate on patient care. Patients will value the upfront clarity about their financial responsibilities, leading to a positive experience.

Why clarity billing
Our commitment remains unwavering until our clients' satisfaction is fully attained.

Submitting clean
claims
Increasing your
revenue

Reduce denials


